What We Do
Minimizing impact, maximizing care with advanced radiation therapy
When faced with an unexpected medical diagnosis, finding the right path forward becomes paramount. Oklahoma CyberKnife is your trusted ally, providing the information and personalized guidance you need to make confident decisions.
Seeking an alternative to traditional surgery? Worried about the potential effects of radiation on healthy tissue? Curious about how CyberKnife® technology can minimize disruptions to your daily routine? Count on us to help you uncover a treatment plan tailored to your unique circumstances.
With access to cutting-edge technology and a team of dedicated professionals specializing in advanced radiation therapy, we prioritize compassionate care to ensure a comfortable journey. Reach out to the Oklahoma CyberKnife team today to discuss your situation and explore the possibilities together.
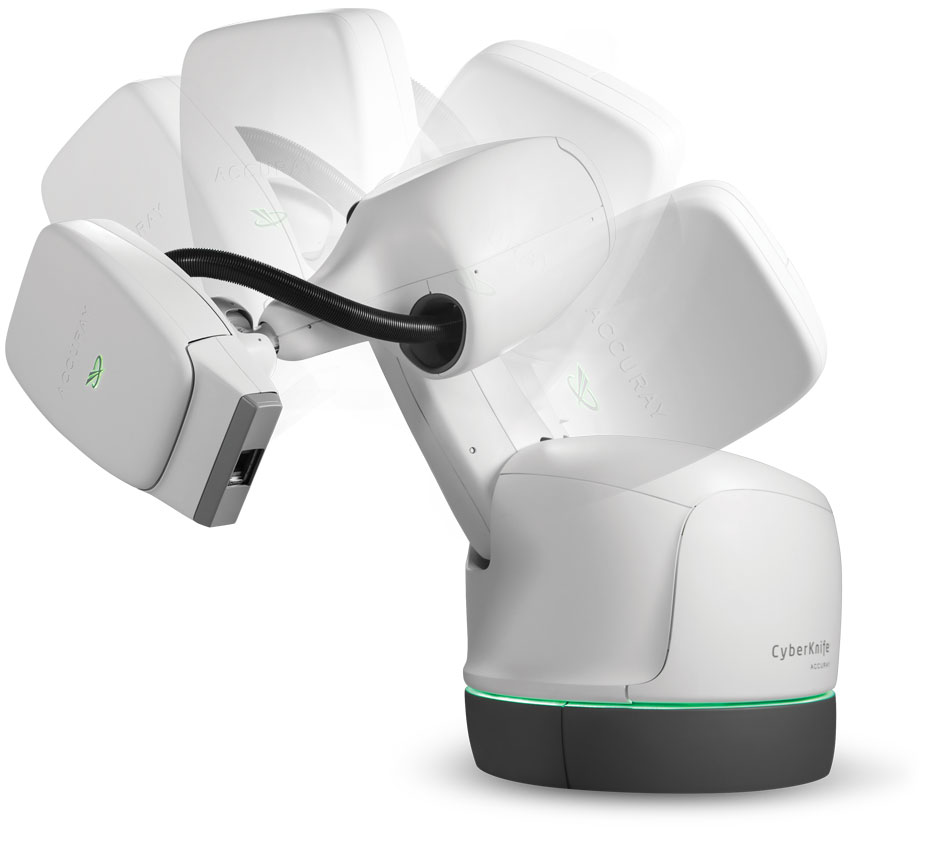
Our Technology
CyberKnife precision delivers a number of unique benefits to patients
Proven Therapy
FDA-approved to treat any part of the body
Safer Treatment
No incisions, anesthesia or hospitalization
Shorter program
1 to 5 visits lasting less than one hour each
Precision Targeted
Surrounding healthy tissues exposed to less radiation


 Diane Heaton, MD
Diane Heaton, MD Connie Nguyen, MD
Connie Nguyen, MD Cynthia Bryant, MD
Cynthia Bryant, MD Barbara Barrick, RTT
Barbara Barrick, RTT Kelsey Lovett, RTT
Kelsey Lovett, RTT Tyler Collums, PhD, DABR
Tyler Collums, PhD, DABR

